|
For too long, men - fathers, sons and brothers - have learnt that it’s better to suppress than express. Emotions, especially vulnerable ones, have been tightly wrapped up in our high-vis shirts and deemed ‘too weak, too feminine or too sensitive’.
Understandably, cultural issues have played a role in this experience. Generations of men being absent through the impact of war and work have taken a toll. Under-fathered boys have been taught through the rough and tumble of homes and schools that to survive you have to be tough, strong and competitive. The old adage that ‘being vulnerable is being weak’ still pervades.
It’s an interesting time for men. We are deconstructing ourselves through our desires to be more nurturing and present in our families, whilst feeling bookended by the essential needs of our woman and community to be healthy and non-violent. Somewhere in this mix, we’re pioneering a new wave of masculinity, and we need too.
In my experience, many men are isolated. Men can seem to lose sight of their friendships and networks either through being too shutdown or too overwhelmed. And yet, Most men I meet desire more connection; more time together outside of the pub, where they can unwind the layers of conditioning and find our core. Working with men and on my own masculinity for over 15 years, the future is clear, claiming our vulnerability becomes obvious. And why not? It take a good dose of manly traits to to do a full suite of our emotions. Courage, strength, determination, focus, to name a few. Men can bring all of their masculinity to their vulnerability. I know, I’ve learnt through my own journey the cost of suppression and the impact this can have on my health, relationships and work life. So where do we start? Courage. It’s all about taking a risk really. Sometimes it’s as simple as picking up the phone and dialling a friend. Trying something other than the beer and BBQ culture, like kicking a footy around, hitting a bike trail or meeting on the beach. Sometimes, it’s about telling your partner something more about what we are feeling other than ‘i’m frustrated, tired or i don’t know’. And sometimes it not that simple. Because we may need to upgrade some skills, build some more resources and ultimately get ourselves a better emotional tool kit. We may need to rely on not only our courage, but also our determination, making those appointments to see a health professional or joining a group with other men who are also wanting transformation. And of course, we need focus. A focus to not give up, to push past the inevitable uncertainty. To find the strength to stand in the fire, face the fear and find a new version of our manhood. In essence, I'm talking about connection. When I really look into my needs, I keep facing the realisation that there is a power in sharing my experience, where I can be seen and can belong in a more real version of myself. As men, when we can create these more intimate connections, we can start to action a transformation of our masculinity, healing the past generations of wounded men, and raising boys and girls that know men can have a heart and a backbone. Check out my latest podcast “The Strength in Vulnerability” below. Author and podcast producer: Sean Tonnet. You can also check out Sean's other podcasts here.
0 Comments
A new year's gift to Mothers everywhere. In this episode of Pregnancy, Birth and Beyond, we are speaking with Dr Marion Rose, passionate about supporting mothers and babies, Marion’s unique methods have helped thousands of families in feeling more connected, compassionate, present and loving in their relationships. Supporting women to reconnect with their true loving nature as a mother and supporting mothers in helping their child stay connected with their connected, compassionate and cooperative self form the bedrock of her work. Marion has a 30 year background in developmental psychology and psychospiritual psychotherapy, with a Ph.D. from Cambridge University. She has been a University Research Fellow in infant development and has taught The Therapeutic Relationship to M.A. students. Through her work, she has been supporting mothers with pregnancy, birth and parenting since 2001, becoming an Aware Parenting Instructor in 2005. Marion has two children a 16 year old daughter and an 11 year old son and is a sister mother to two beautiful twins. First aired on 99.9BayFM in Byron Bay, Australia on December 17th, 2018. Produced and presented by Annalee Atia with Guest Dr Marion Rose. For more information about Marion's work head to www.marionrose.net 
PBB Media
Contemporary Conversations where Stories, Science, Traditions and New Ideas meet. www.pbbmedia.org Copyright PBB Media, Annalee Atia and Dr Marion Rose 2018
This month we feature a special article from Dr John Travis, MD, whose career has had him realise "the currency of wellness is connection". Here he speaks on the strains that can emerge with family during the emotionally charged festive season, and how we can see these as opportunities for growth.
It’s the people closest to you that can drive you nuts—especially with the increased contact during so-called festive times. Not only might you painfully compare yourself with the culture’s idealised relationships promoted by the media and Facebook, but the increased time that you’re getting reflections of your own shadow from those closest to you can be taxing.
A key concept in wellness is “owning your projections will increase your connections.” Owning our projections requires confronting the deeply embedded cultural conditioning that we carry from early infancy. We are conditioned to find someone/thing to blame for our problems, along with suppressing our inner feelings. Deconditioning ourselves is the ultimate test of resilience, and relies on our recently discovered neuroplasticity. Owning our projections is the key to taking full responsibility for ourselves and experiencing more self-love. It’s also a great shame-voider. Our shadow contains the opposite of all of those qualities that we define ourselves to be (“a caring person,” “a careless person,” etc.). “Within the appearance is its opposite.” We project both our dark shadow (criticising/blaming), and our light shadow (admiring/idolising) and until we own every aspect of ourselves, light and dark, we’ll continue to project them onto others, thereby decreasing our ability to connect. Thus learning to “eat” of our shadow brings liberation from shame and greater connection. In summary:
Resources “Shadow-Work-Guide.pdf”; “Psychological-Projection-Guide.pdf”--ScottJeffrey.com, Non-violent CommunicationCNVC.org, Byron Katie--TheWork.com The Five-Minute Relationship Repair--SusanCampbell.com Re-evaluation Counseling (Co-counseling)--RC.org For more exploration of our shadows, and how to deal with them, catch our interview with Dr John Travis in this podcast (below).
We also spoke with Dr Travis earlier this year about how our shadows can show up during times of enormous personal change, such as when a baby arrives. Catch that interview here (below).
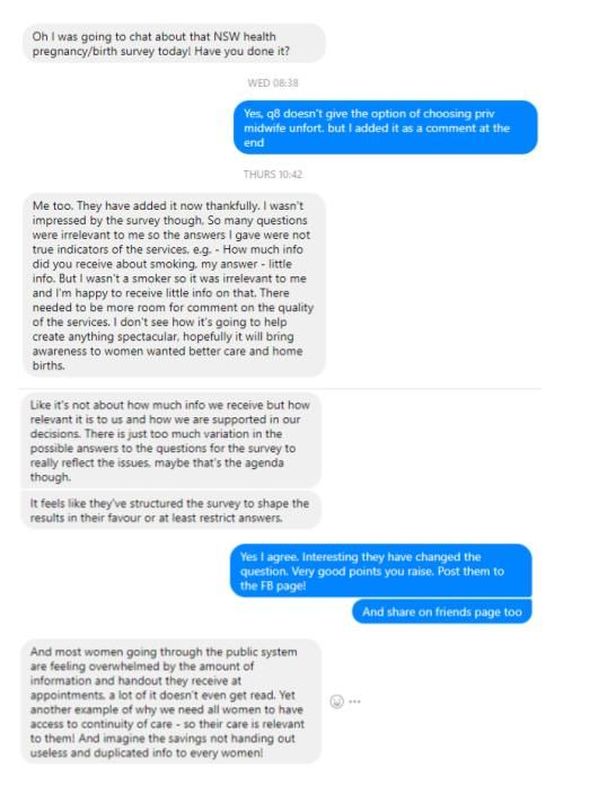
Earlier this week NSW Health published an online survey "Maternity care in NSW: What's important for you?" for families who had had a baby in the past 10 years. On their Facebook page NSW Health stated they are "reviewing the maternity care policy and want to hear what’s most important in your experience".
The survey has sparked lots of interest in six days it has been out - in large part to the lack of the option of independent midwife in Question 8 for the type of care received. While mother of three and consumer advocate from Tamworth NSW, Samantha Wibberley, agrees with this shortcoming, she sees a series of other problems with this survey that will limit the amount of information NSW Health stands to glean from its consumers.
Samantha and I exchanged these messages yesterday morning in between shopping and dropping kids off (my responses are in blue).
Samantha had a good mind to write an article "picking apart" the survey but in this fast-moving online world and three kids under six to juggle, how's a mum to get time for that?? I don't know how she does it all, but like her, I was keen to seize the moment, so we made time for a quick recorded chat yesterday afternoon about it to share with you now. (Click link below.)
Samantha has since added that she's really happy to see the "survey being shared with so many people and that consumers are actively engaging with NSW health and wanting to provide their feedback, I hope more women continue to do so and keep on demanding a service that meets their needs. We deserve that!"
She would also like to know if NSW Health had consulted with a advisory group with consumer reps when they developed the survey. I'd love to know that too! Samantha has been advocating for the women of her region for 18 months now, since the closure of the Midwifery Group Practice at Tamworth in April 2018. She and the women of that region stepped up to have their voices heard and the MGP has been reinstated (in a manner of speaking) and a maternity services committee with consumer representation has been established to improve the services there. You can connect with Samantha and her community's campaign at Friends of Tamworth Maternity Services in Facebook. You can also hear about the early part of Samantha's work in this podcast (which also features two other women's struggles with their local health services).
Our thanks to Samantha for sharing her thoughts and being willing to bring them to an open forum, and to NSW Health for starting the conversation! We'd love to engage with NSW Health more! We have much to be proud of with the quality of care that can be found within NSW Health, but they could do so much better with more consultation. And we'd love to help with that process.
If you have comments you'd love to share about your maternity care, or this survey, you can email us at hello@pbbmedia.org. ~ Sally Cusack
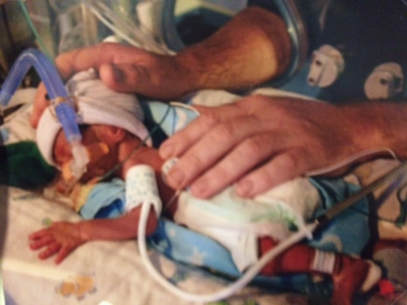
This morning my sister sent me a #NICUAwarenessMonth video on social media (NICU - Neonatal Intensive Care Unit). It shows women with their premmie babies in the intensive care unit. The music is powerful and the words inspiring:
”This is not what you pictured... your baby surrounded by machines and wires... leaving the hospital empty-handed... But you are strong.. Because your baby needs you... To comfort them even when glass separates you... This journey is overwhelming... But you are adapting.” Nine years ago I had a premmie baby. I had pre-eclampsia which resulted in my son being born two months early via emergency caesarean. He weighed 835 grams. We had gone for an impromptu check-up and didn’t come home for two months. Most of that time we spent in NICU. That baby has grown into a wise, creative, funny, resourceful, intelligent and beautiful little boy. We are so blessed. And yet, as I sat at the table with my morning coffee, watching this video, tears poured down my cheeks. It caught me off guard. Again. This mountain of feeling - so mixed with grief, love, traumatic memories, gratitude, and even a bit of shock, all these years later. The endless helplessness and shock. The survivor guilt - so many people so much worse off. The babies that didn’t make it.
And I’ve done a lot of work on this already. Am accustomed to deep self enquiry.
So how to survive NICU? My son is thriving. He has flourished since his first breath, though we all fought harder than we ever expected to. We focussed everything on him. That habit was hard to break. Time has offered its mellowing gift. Six years ago we had another beautiful son, also birthed in fairly dramatic fashion. These days we are getting on with the business of living. But it took quite a few years for us to find our feet. More than I expected. We were deeply impacted by all that happened, and there have been lots of challenges along the way.
When I think of that time, my greatest support is the bone deep certainty that we did everything we possibly could to create an environment in which our baby could thrive, despite the beeping machines, changes of staff and invasive procedures. We left nothing in the tank. From Kangaroo Cuddles to fierce advocacy. We held firm to our convictions around attachment parenting, despite the dominant culture.
This claiming of our parenting style in the midst of an environment less than conducive to an intimate connected family circle, helped to ensure our role in a setting where we could easily have felt extraneous. One of us was with our baby 24 hours a day, just as it would have been if we were home. I sang lullabies through the glass. We even put up little signs on the humidicrib asking people to speak respectfully to/about him. Some staff loved us, some not so much. For someone who is a bit of a people-pleaser, that was surprisingly OK. I let my Tiger-Mama do her thing when necessary. If we had listened to the dominant culture, then and later, there may have been a very different outcome. In essence, we shaped the situation in any way we could, in a situation where so much was completely out of our control. One of the offshoots now, is that other people’s opinions about our parenting don’t matter so much. Under the layers of shock, we found a deep sense of agency that has seen us through our parenting to date. We learned to trust ourselves and trust our kids. I have come to see that the important question isn’t “How was the birth?” But rather, “How have you been transformed by motherhood or fatherhood?”
This processing of our experience has been hard-earned and is ongoing. There is a whole lot of isolation that comes from such an extra-ordinary experience. It’s not great coffee shop conversation. No-one really knows what to say to you. And it can be tricky to integrate into the “Mums and Bubs” set with such vastly different formative stories. I didn’t talk much to other people in the beginning. It was hard to reconcile my experience with what I presumed theirs had been. A surprising number of friends dropped away. I was so insular, both out of my own trauma and the reality of needing to protect my vulnerable baby. It seemed like there was no way anyone could connect with me in the enormity of all that had happened. And I was too exhausted and focussed on survival to try. I wish that I had kept talking, taking the risk to be heard, had kept going until I found the support I needed.
I’ve come to a place, finally, where I am ready to be heard. To be witnessed. For someone to stand present with everything I say and not feel compelled to compare it to something they’ve heard or experienced. To not try to make it better. Just to listen. I’ve discovered my own need to stop protecting other people from my story and to have the courage to just tell it. There’s a surprising amount of fresh air in the places left by the telling.
You can listen to Krishna's interview with Sally via this link below.
Mandala Diehl is director of Federal Children’s Community Centre in northern NSW and a childhood educator. Over years she watched an overrun piece of land grow thick with lantana and had a vision for change: she would create a living classroom – a bush tucker garden for the children to learn about nature, to appreciate nature and to be in nature.
Together with a local bush regeneration expert and the Widjibull elders (on whose land the garden stands) they created an astonishingly beautiful garden that thrives today. This is more than just a bushtucker garden. It’s a living, breathing classroom that teaches children about bush foods, plants and local animals. It also works to forge a bridge between the indigenous community and it’s white inhabitants.
People visit to sit in the beauty of it’s nature, they come to learn how to replant the native plants that belong to this region, and they begin to understand the impacts of working with the ecosystem of the Widjabul land. Animals are returning, the soil is nurtured and the community tie is strong. Today anyone can enjoy the space; come together and learn about this living classroom. Federal Community Children’s centre is also thriving. Under the nurturing care and tutelage of a bunch of remarkably passionate educators, each child’s individuality is celebrated. The kids spend swathes of each day outdoors in child-led play, and in this garden. Come and visit sometime. It’s worth the short drive.
Author and Podcast Producer: Kimberley Lipschus
It is not our differences that divide us; it is our inability to recognise, accept and celebrate those differences.
Audre Lorde
Every human being on the planet is born an individual; there is not a finger print on a single hand that is the same. Yet, in 2018, we live in culture that holds a candle to conformity. When this becomes the dynamic, for those who are different, it can be a dangerous time to be on the planet.
Segregation, exclusion, judgement. But what is it to feel different? Perhaps you live with a disability: physical, sensory, psychiatric, neurological, cognitive and intellectual. Others may feel they stand out for entirely different reasons – race, ethnicity, religious belief, sexual persuasion. Even political beliefs can set someone apart. Whatever the reason a person stands out from the crowd, no one deserves exclusion. Everyone deserves to experience it’s opposite – inclusion. Misa Alexander’s middle son, Hugo, lives with mild autism and an intellectual disability. In the playground Misa would watch other children regard his behaviours – which included shrieking and spinning - with curiosity. She watched her son’s exclusion from play, from friendships. She saw a trajectory of exclusion spreading out before her son and a fire ignited within her. It started with a flyer in the pockets of all parents in Hugo’s pre-school. This is my son, she told them. This is how he may act throughout the day, and this is why he acts this way. It worked. The parents talked to their children and slowly, Hugo’s life of inclusion began.
But more was needed. She collaborated with author, Erin Knutt, and together they created Fergus and Delilah, which Misa illustrated. The book turned into a website, and the website became a tool kit that any school or educator can use.
Today Hugo attends a public school, and his mother is a full time Inclusion Advocate, not just for her son, but for anyone who stands out from the crowd. Surely all of us should seek to stand out? Stand out for what we believe, for who we love and for who are. Teach our children to celebrate difference in others as well as themeselves. Wouldn’t it be lovely to have Misa proudly declare that she’s out of a job? We think so.
Author and Podcast Producer: Kimberley Lipschus
In this episode of Pregnancy, Birth and Beyond, we are discussing Gratitude, Gathering and the power of storing positive experiences in building true resilience, a more positive outlook on life and a whole suite of additional benefits! Dr Lauren Tober, a Clinical Psychologist, Life Coach and Yoga Teacher based in the Byron Shire is with us in the studio, she is the founder of acclaimed photographic happiness project Capturing Gratitude and runs a heart-centred practice in Mullumbimby - the Centre for Mind Body Wellness, where a gorgeous array of practitioners supports individuals in the local community to lead a life of wholeness, happiness, health and authenticity. Listen to our celebration of World Gratitude Day, in the podcast below.
we must see that it is not happiness that makes us grateful, but gratefulness that makes us happy Join the Gratitude movement!
Capturing Gratitude is a global photographic happiness project founded by Clinical Psychologist Dr Lauren Tober, with the lofty goal of increasing worldwide happiness. The research is clear, a daily gratitude practice increases our physical and emotional health. And sharing our gratitude spreads the joy even wider. The idea behind Capturing Gratitude is simple. Pause throughout the day to take photographs of things you’re grateful for, then share them online to create a ripple effect around the world.
Dr Lauren Tober, a Clinical Psychologist, Yoga Teacher and Gratitude Photographer based in the small town of Mullumbimby Australia, stumbled upon gratitude photography by accident. After ditching her DSLR for her iPhone camera one day, Lauren started taking photos of things she was grateful for, just for fun. But Lauren felt the effects of this simple gratitude practice immediately. “I started radiating happiness almost right away” she says. “I thought gratitude photography would be a fun creative project, I had no idea the profound effect it would have on my own happiness and those around me!” And the research is backing up Dr Lauren’s experience. Robert Emmons, one of the world’s most prominent gratitude researchers has found that a short and simple gratitude practice has far reaching effects on both our emotional and physical health. In an early gratitude study, Emmons and McCullough asked hundreds of individuals to either record things they were grateful for, record hassles from their daily life or simply record any events that had affected them (2003)1. In a series of studies with hundreds of participants, they found that those who had been randomly assigned to the gratitude condition:
Not bad for a simple shift in focus! More recently, Rash, Matsuba and Prkachin (2011) found that grateful contemplation resulted in increased physiological coherence, suggesting increased activation of the parasympathetic nervous system (the relaxation response) and decreased activation of the sympathetic nervous system (the stress response)2. Their research indicated that being grateful reduces stress and increases wellbeing. All the gratitude research to date has confirmed what we already know, that counting our blessings is good for us, and those around us. Nobody sums this research up better than Brother David Steindl-Rast, who says “we must see that it is not happiness that makes us grateful, but gratefulness that makes us happy.” Tips for taking in the good with Rick Hanson.
Lauren and I discussed the work of Rick Hanson's on the podcast, below is a wonderful intro to what he is all about. His books mentioned were Resilient and Just One Thing. You can listen to Lauren's interview with Rick here and more like it on her website.
Consent is on everyone's lips. From media discussion about 'enthusiastic consent' in sexual encounters to medical requirements for 'informed consent', it seems pretty clear there is a problem with 'consent'. If consent was what mattered, we would not need to prefix it with a qualifier. Consent is about freeing someone of liability. To seek consent is to clearly express a desire for a particular action or outcome. The person seeking consent has the power position. They are placing someone in a position where it is known they are expected to consent. To not consent is to ‘refuse’ or ‘decline’. To not consent can be met with repeated asking – coercion – until consent is relented. It can also be met with increasing pressure and threats. In some situations consenting to ‘step one’ is treated as consent to any subsequent steps. In medicine, it is a legal requirement to obtain ‘Informed consent’. The legal role of the person seeking consent is to provide full disclosure of the procedure…and any subsequent ones that may arise. In maternity care, this consent is often sort at the critical moment, under intense stress and pressure. The ‘informed’ component means “I told you what I was legally required to” not “you know all you need to know to decide what is right for you”. It does not mean all options were understood or available. When it comes to pregnancy and birth, it is possible avoid this situation. This means considering various possibilities in advance, and taking the time to look at the risks and benefits of different options and make an informed decision about the direction to go. So if ‘consent’ is requested it can be given as actual informed consent, or confidently declined knowing that the decision is valid and based on understanding. Reflecting on that, replace ‘consent’ with ‘decision’ and the implied yes is removed. The person seeking consent may still recommend, assume or prefer a particular outcome, but when framed as a decision the other possible outcomes become visible. With ‘consent’, only one outcome is spotlighted. This simple shift in language may just be the key to helping reduce birth trauma. Above image by Rawpixel on Unsplash.com.
As a midwife, I face the enormous and important task of educating women and families on pregnancy, birth and the early days of parenting. Because a woman’s care is often fragmented and she may see a different midwife or care provider at every appointment, it is very difficult to ensure we are providing all the information and knowledge that a mother is deserved so she can make informed decisions throughout her care. A study in 2010, ‘Queensland Centre for Mothers and Babies: Having a Baby in Queensland', states that in their study of over 3500 women, 70% of women who had an epidural felt uninformed or did not provide consent to the procedure. They also stated 26% of women had not been informed or consented to their episiotomies. As midwives, how can we better ensure women are involved in their care and informed appropriately? I have worked in several models of care, and in my experience, the model of care that can provide the most thorough and informative education, and therefore true informed consent from women, is that of a model where there is continuity such as a midwifery group practice or through a private midwife (look out for our radio podcast all about Privately Practising Midwives in August). When we work in a model of care where there is not continuity, as midwives, we must really make sure that the women we see receive all the information they need and are actively involved in their care. We must know that the decisions they make are based on INFORMED consent. We have a responsibility and duty of care to keep women and babies safe, and they have a right to be respected and not coerced in their decisions. Sometimes women make an informed decision that goes against routine or recommended care- they may decline a routine blood test or ultrasound, or decline administration of antibiotics for GBS. We must make sure we find out why she declines, as a woman declining electronic fetal monitoring in labour, may not be opposed to monitoring, but she may be concerned about mobility in labour. We can better understand her needs by asking questions and respecting her right to make her own decisions. Top photo by Brandi Redd on Unsplash.  Author Danie Smallwood, Midwife and PBB Media Contributor I am a midwife and I am a mother to a delightful little toddler. For the last 6 years I have worked in various locations as a midwife, and informed consent has been an important part of my practice. It is a woman’s right to have autonomy over her body and her baby at all times, and I am legally obliged to discuss the benefits and risks of any procedures or treatments with the women I care for. As a midwife, informed consent is about providing information, offering alternatives, encouraging questions and working together with a woman about her decisions and care. I knew that becoming a mother would involve a lot of decisions; decisions that I have helped many women make in my years as a midwife. It felt very different to be on the other side of decision-making, rather than on the side of providing information and knowledge. As a mother, Informed consent involved knowing my rights, gathering the information, understanding this information and giving my permission for something to happen, before it happens. During my pregnancy, I was fortunate to be accepted into a low risk birthing centre for continuous care by a known midwife. This enabled me to develop a trusting relationship with my midwife, and feel safe and supported in the decisions I would make for myself and my baby. I also trusted in the knowledge she shared and that with many months of mutual discussions, she would know how to support me and my choices when it came time to labour and birth. Informed consent in my pregnancy involved asking lots of questions and seeking further education. It involved plenty of listening and lots of reading. Some of the decisions I needed to make could be made based on the knowledge I already had as a midwife, but the knowledge and decisions were now a lot more important because they also involved my unborn baby. Something that helped me in decision-making, and something that I offer all women is the BRAINS anagram. This is a valuable tool to have when confronted with an important decision, and can guide you in your discussions with your partner and/or care provider. B- Benefits: What are the benefits to this procedure/test? R- Risks: What are the risks associated with this procedure/test? A- Alternatives: What are the alternatives to this procedure/test? I- Intuition: What does your intuition tell you? Does the information make sense? N- Nothing: What if we do nothing/decline this procedure/test? S- ‘Scuse me: Take some time to discuss your options and make your decision. S can also suggest the need for a second opinion if you require. By 42 weeks pregnant, my baby had not arrived yet, and my care was handed over to a larger hospital, now without my known midwife by my side. I was armed with my birth plan, outlining my preferences. I was fortunate that a lovely doctor and colleague of mine was on call that night and he took the time to talk through the decisions we needed to make, many of which I had not expected to make in my birth story. I felt educated when I provided consent to procedures, and felt supported in the decisions I made where I declined consent. My baby was born after a long and challenging labour, but I felt empowered because I knew I had educated myself, made important and informed decisions and because I felt respected in the choices I made. I was the key decision maker in my story. If you have recently birthed, did you feel you were given adequate information from our care giver so you could make the best decisions for you and your family? Or were you rushed into making decisions that you now feel unsure of? We would love to hear from you at hello@pbbmedia.org. If you would like to read more about informed consent and your rights, check out these links fromHumanRightsinChildbirth.org, MyBodyMyBaby.com.au, Birthrights.org.uk. And we discuss consent in this podcast: As Long as the Baby is Healthy Part 1 (Photo by Jason Blackeye and Unsplash)
You have been on an incredible journey throughout your pregnancy and giving birth to your new baby. In fact, this has been a rite of passage where you yourself have moved through a transformation of your own and in a sense have been re-birthed from Maiden to Mother in your own life. The first weeks, months & even years after birth, is a very sacred time for you and your baby. In, many ancient traditions it is highly recommended for mother and baby to stay at home being cared for by family and friends at least for the first 40 days or longer. During this time, the mother can rest and is fed nourishing foods to sustain her while she recovers from the birth, and conserves her energy for the many hours of feeding and caring for her new baby. If a mother is breastfeeding, it is also important that the new mum is kept hydrated while her body is busy producing litres of milk for her baby every day. In indigenous or ancient cultures women probably birthed mainly in nature such as a quiet forest, cave, waterhole or lake where she felt safe and secure. As civilizations developed women began birthing in designed space for women menstruating and birthing such as a “Red Tent”, or “Moon Hut”. Here she would stay until she felt fully recovered from the birth and was ready to venture back out into the world and resume her usual daily activities and responsibilities. For some women this may have been 4 – 6 weeks & for other women perhaps, 4 – 6 months depending on how the birth unfolded and her health and resilience in this post birth period. For most of us, we don't have the luxury of being cared for ‘hand & foot” 24 hours around the clock, however, there are some ways to create our own Red Tent in your home and living spaces.
Within your home or private space, you may call in support from your partner, family friends, the community, healers and other professionals. This may be an attitude that you need to develop if you are not accustomed to asking for help or reaching out for assistance. However, this is a wonderful skill to develop early on in motherhood as it will help sustain you over the many years of mothering, so that you can receive as you give to your child or children. This receiving may be anything from someone making you o cup of tea or a meal, getting a massage, your house cleaned or holding you baby for a 10 minutes while you shower. Importantly, having a support network of people who you can talk with is vital especially for the first 12 months. This generates oxytocin and other feel good hormones, which help establish a healthy mental & physical wellbeing. Establish a Rhythm In the beginning, it may feel like any routine you had while you were pregnant has gone completely out the window! That’s ok and part of the process of re-adjusting to life with your baby. Yes, initially your baby will set the rhythm depending on their sleep and feeding times. Even in these early days, you can still be setting up a routine for yourself, for instance, find a period of time every day you enjoy having a shower or bath, for instance between 9-10am everyday. This time frame will vary depending on you and what feels most relaxing & nourishing. And you can do the same for your meal and sleep times. Find an approximate time for breakfast lunch and dinner, and an ideal bedtime. Eventually, over time your baby will fall into your routine more and more. Nourishing Food After giving birth, your body is in recovery mode for at least the first 3 - 6 months (in fact up to two years!) and during this time, your digestion usually slows down considerably. This means that anything that is already cooked will digest easier, compared to raw food that requires much more effort from the stomach and digestive system to break the food down. Suggested foods are soups, broths, stews & casseroles cooked at lower temperatures, rather than fried or barbequed. Cooking with Ghee (butter heated to remove the milk solids, retaining the precious oil), mild herbs & spices, root vegetables (avoiding ‘gasey’ veg) as well as some animal protein give you the nourishment you need after birth. Even in India where the bulk of the population are Hindu & therefore, vegetarian, Ayurvedic doctors recommend eating chicken & fish during pregnancy & for the months after giving birth. If you don't eat meat, one possibility is to try bone broth or stocks that you can add to any of your dishes without eating the actual meat. Otherwise, include as much protein & oils into your diet as possible as well as supplements such as iron, zinc, B12 and magnesium (Ideal to check with a kinesiologist or naturopath about which supplements are best) Relax your Body Your body has been through many changes throughout the pregnancy, the birth and now as you care for your new baby, possibly spending many hours a day and night feeding, holding & rocking your baby. This means that your body is now working in new ways and holding different positions for long periods of time, such as when you hold or feed your baby, pick your baby up or co-sleep with your baby. There are a number of ways to keep you body soft and relaxed during this time. The first way is with oil massage. In India and other traditional cultures, women after giving birth are massaged daily for up to 3 months or more - can you imagine this ?? How divine! Even 1 massage every week or two is extremely beneficial for you physically and mentally, as a new mum. I invested in a weekly massage after having my second child for the first 10 months. My health and vitality was definitely stronger because of this with my second child, compared to with my first child. In addition to receiving an oil massage, you are able to massage yourself everyday. The Black sesame oil contains beneficial nutrients for your body tissues and especially for strengthening your nervous system. This is best done 20-30 minutes before your bath or shower, focusing on the ears, spine, hips, belly and feet. If practical, it is preferable to leave on as much of the oil as possible. Another easy way to apply oil is to place a teaspoon or 2 in your bath so that your entire body is covered in the oil like a protective coating for your body and nervous system. Like Cleopatra, you can put milk and rose-petals in your bath, to soften your skin, awaken your heart and feel like a goddess. This too is an ancient ayurvedic practice. Yoga, stretching and exercise are other important ways to regularly stretch & release tight muscles and strengthen particularly, pelvic floor, abdominal muscles. You may want to do this at home in your designated space, even 10 minutes a day is enough to keep muscles limber. After the 3-month mark, if you have a local postnatal yoga class especially for mother (ideally with your baby) this can be a great way to gently come back into your body while you connect with other mothers & babies. If you feel like movement that will loosen you up, dancing is a great way to relax your body, shake off your day, feel playful and have fun. Combined with music or your favourite song, dancing can take you out of your mind, your tiredness and into world of rhythm, ecstasy and another time & space. Get Sexy Yes girls, you read this right! Only when you feel ready … find ways to feel sensual and re-connect with your sexual energy (sometimes referred to as Shakti). This might simply be putting on a dress that makes you feel beautiful and sexy. Being creative helps to re-nourish yourself and generate your Shakti. Or having a bubble bath, giving yourself a pedicure and a home-made facial. Organising date nights with your partner is not only fun, it is important to stayed connected as woman and man, not just as mother & father to your child or children. You are giving many hours of each day, so allow yourself to regularly receive massage and/or loving touch from your partner. Simple Self-Care meditation Within the first 30-60 minutes of waking, find time for yourself to sit, or lie down if you wont fall asleep. (Ideally in the sacred space you have created for yourself). This meditation can be anywhere from 5 to 20 minutes or more. You may even do this while you are feeding or holding your baby. However, if you find it difficult to concentrate and focus on yourself then it may be best to do this on your own while your child or children are sleeping or cared for by another. It may be that you need to pre-book this time in with your partner or family, so that they know to expect this as part of your daily routine. Close your eyes, follow the rise & fall rhythm of your breath, notice how your body feels all the way from your toes to the top of your head. Once you feel settled... you may put your hand on your belly & connect with your womb space. If you prefer hands in a yoni mudra go for it or ok if not. Then ask yourself "what do I need for myself today?" The answers may seem simple or ordinary such as '20 minutes to myself', 'a swim in the ocean' or perhaps something deeper such as "a change of job or career', 'a holiday' or 'letting go of a relationship'. Trust what comes to mind. Stay here as long as you need to connect with your needs for that day. When you are ready to come out of the meditation, be aware of your body sensations, breathing, your 5 senses taking in your experience and being back in the current time and place. When you feel ready, open you eyes and stretch out. You may want to write down what came to you on a piece of paper to remind you through your day. Alternatively, you could note your meditation and your needs for the day in your journal. It may be interesting to see if there are patterns that emerge over the following weeks, months or years so that you become familiar with your basic needs to keep you balanced, happy & healthy.
I know when I became a mother, I changed, and in a good way. I was the same person with the same face, the same history, the same story but something was different. The word ineffable reflects the metamorphosis that occurs when a woman (or person) becomes a parent. It is hard to put into words the profound shift in identity and purpose that happens when you give birth and slowly grow into motherhood. My guest Kari says in this interview “you don't wake up a mother, it is something you grow into.”
When you become a parent, pre-birth expectations drop away as reality kicks in. Life that perhaps was once goal or career orientated shifts as life with a baby forces a new daily rhythm. A slowing down, surrendering and letting go for a new way of being in the world. 
My guest Kari Azuma, leadership development coach and mother, from Santa Barbara, California joins us in a conversation about her transition to motherhood, birth as an opportunity for personal evolution and finding your passion and power as a mother.
This episode focuses the lens on motherhood; my guest Kari specifically works with mothers. Yet, whatever gender you identify as this episode speaks to all parents in the metamorphosis that occurs with the birth of a new family member.
I ask Kari about her reality post having her baby. What it means to slow down. There is a notion of six weeks postpartum and then you go back to your pre-pregnancy self, back to your pre-pregnancy clothes, job, sex life and interests as if you never had a baby. This concept intersects with being measured up against your pre-child state and your new life with a baby or young children. You can't always go at the same pace or speed at which you once could and you are not always interested in the things you once were. Part of pregnancy and the journey to becoming a mother involves dreaming and planing, what life will be like with your baby. I ask Kari, about her pre-birth expectations of life with a baby and what a more truer perspective of becoming a mother is. Kari says “one thing you can count on, is that there are unknowns. To know that life isn't going to be a straight line. Have a plan and be open to the mystery of becoming a mother.” Sometimes birth doesn't go to plan, despite how much preparation and planning happens. Kari, mentioned her birth was a traumatic experience. I wanted to know more about her experience and how it has shaped and changed her perspective on life, work and herself. More covered in this episode: Postnatal depression. Motherhood as a powerful opportunity for transformation. Birth as a Rite of Passage and the commercialism of motherhood Take a listen to our interview with Kari Azuma here:
I don't know about you, but subconsciously I've been looking for this word - matrescence - and the social movement it will bring, for a long time.
Matrescence is the "time of mother-becoming", as defined by anthropologist, Dana Rafael back in the 1970's in her essay "Matrescence, Becoming a Mother, A New/Old Rite de passage". How is it this much needed term has taken so long to enter common parlance? Why is it when pregnant, we don't speak of ourselves as 'going through matrescence' and spend our pregnancy preparing for this great transition when the baby arrives? Feminist motherhood writers such as Andrea O'Reilly would have a lot to say on the reasons behind this, but in this piece, I'm keen to simply be a part of raising awareness of the term matrescence. Why? Once we have a name for an issue, it makes it so much easier to start addressing it.
Dr Oscar Serrallach holds a similar passion for raising awareness of matrescence and the need for support for it, because he sees most women across multiple generations have suffered from a lack of awareness, and therefore a lack of support for this profound transformation of women.
Oscar got involved in this work through witnessing Caroline, his partner and mother to his three children, go through her own transformation and subsequent depletion of her health. He also saw mothers coming through through his medical practice literally worn down to a mere shadow of their former selves by the hardship of insufficiently supported parenting. This wearing down we have witnessed in mothers of young children, and perhaps experienced in ourselves, leads to years of depletion, "postnatal depletion" as Oscar calls it, where a woman suffers physically, mentally, emotionally, creatively, spiritually. "Like adolescence, matrescence needs support" says Oscar. This transitional period holds within it the potential for a woman to forge a new identity for herself and gain new insights in the world and her place in it. However to achieve fully fledged motherhood, a woman needs time and support to integrate her birthing and postnatal experiences into her new role. Catch my interview with Oscar about Matrescence and postnatal depletion below. Hormonal Psychiatry
The only part of my interview that couldn't fit into our national network podcast is Oscar's discussion of hormonal psychiatry, a burgeoning field that practitioners such as Dr Kelly Brogan are championing. Oscar cited a study of four severely depressed postnatal women who experienced rapid recovery after a 60 hour infusion of Brexanolone, which is related to the hormone allopregnanolone. This hormone is produced by the placenta, along with more than 200 hormones, and gaining a lot of interest in circles where perinatal depression is being researched and treated.
Podcast references
Other references on the changes that occur during Matrescence
Oscar also discusses the "massive upgrade" that happens to women's brains as a result of pregnancy, birth and the postpartum period, and some of the research for this is listed below.
By Sally Cusack
Are you a healthcare services consumer? Specifically - have you accessed any form of maternity healthcare services in the last few years?
On Friday May 25th 2018, Sally Cusack & I spent the day up at Tweed Heads, attending a Consultation workshop as part of the governments plans to develop a National Strategic Approach to Maternity Services. The consultation was hosted by the Australian Health Ministers Advisory Council (AHMAC). The expected outcome for the NSAMS project is a document to guide national maternity services policy. Along with about 20 other people we debated and discussed, listened and contributed to the conversation. What should maternity services look like in the future? What are the main frameworks and who are the key stakeholders? What’s missing from the current system and how do we go about attaining a system that delivers better outcomes for mothers, their babies, their families and those that work within these systems? I have the beautiful Sally Cusack in the studio, join us as we discuss all this and more on this special episode of Pregnancy, Birth & Beyond. Listen to the PodcastDefinitions and Links
The following definitions are taken from the Health Consumers NSW website. Visit their site for more information about consumer engagement.
Health Consumer Health Consumers are people who use health services, as well as their family and carers. This includes people who have used a health service in the past or who could potentially use the service in the future. Maternity Consumer Advocate A health consumer representative is a health consumer who has taken up a specific role to provide advice on behalf of consumers, with the overall aim of improving health care. A consumer representative is often a consumer member of a committee, project or event who voices consumer perspectives and takes part in decision making on behalf of consumers. A health consumer representative may be nominated by and accountable to, a consumer organisation. Usually the role is working with a health service (or consumer organisation) and is often in a volunteer capacity. Sometimes the role comes with a small payment to cover the consumer’s costs. About this Episode
Copyright
PBB Media Producer/Host: Annalee Atia Interviewee: Sally Cusack |
Details
NE PLUS ULTRA
AuthorsThe authors of this segment are varied, each post will indicate the author of that particular post. For more information about our team, visit here Archives
February 2019
Categories |























 RSS Feed
RSS Feed